What Makes Your Skin More Susceptible to Pigmentation?
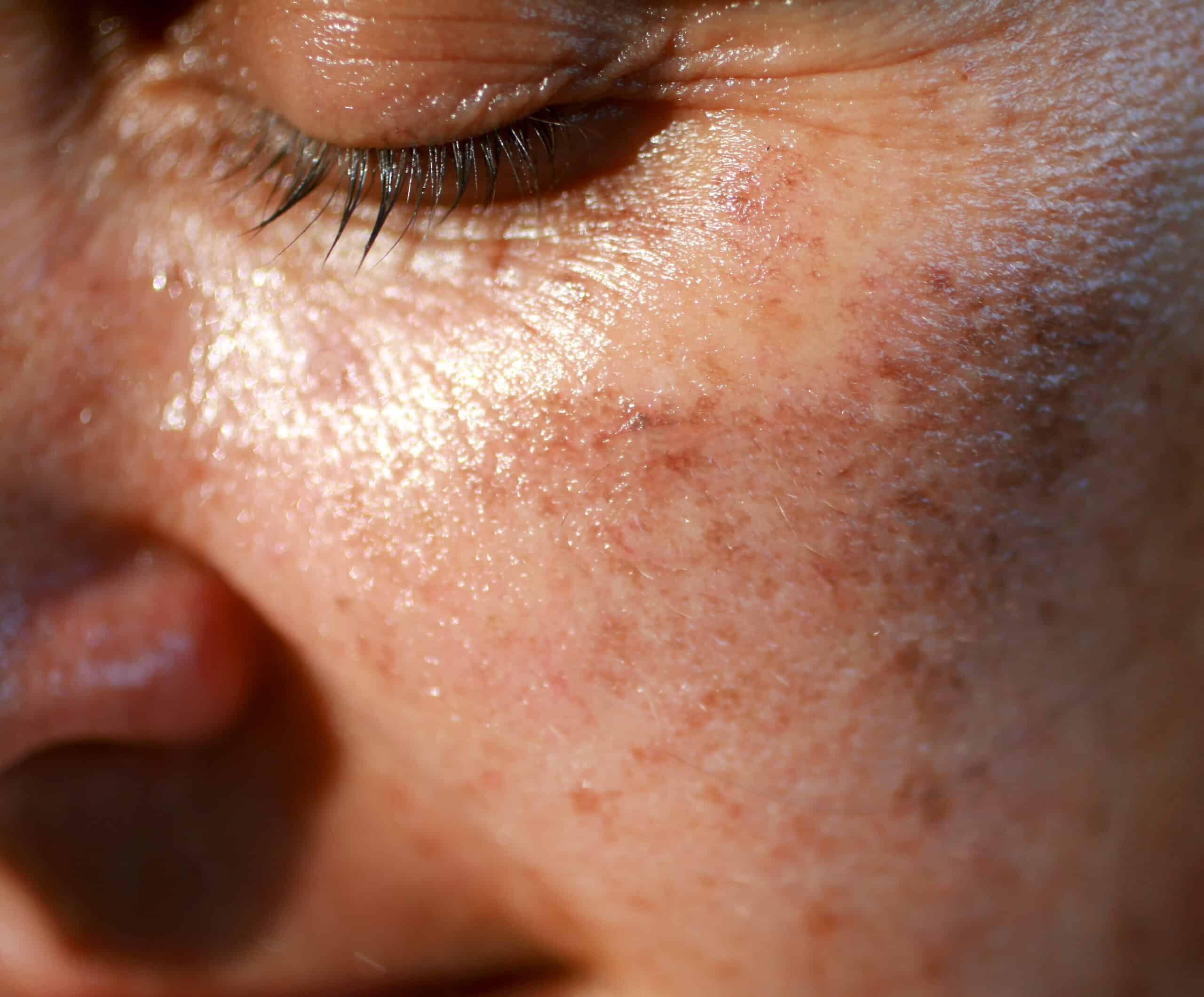

In modern day Singapore, where flawless selfies are highly valued, skin hyperpigmentation emerges as a growing concern as it stands out as a silent reminder of our skin’s often sub-optimal past. These dark spots are often the consequence of previous sun exposure, hormonal changes, or past skin insults and are also commonly contributed by our own genetic predisposition.
In this piece, we will address why some individuals develop hyperpigmentation, while others remain unaffected despite seemingly similar conditions and lifestyles.
Let’s explore the complexities of hyperpigmentation and investigate the factors that make your skin particularly prone to these pigmentary variations. We will also share pigmentation removal options you can consider to treat pigmentation and improve your skin condition.
Melanin is produced in Melanosomes, which are tiny organelles found in cells (Melanocytes) which live at the base of the skin’s surface (epidermis).
Melanocytes can be seen as melanin factories. They have long arms (Dendrites) that distribute the Melanosomes to the skin cells in the epidermis above. As such in most normal skin, melanin is not found in the dermis [the layer beneath the epidermis].
Differences in the number, size and grouping of melanosomes in the melanocytes and the surface skin cells lead to ethnic differences in colour.
Hyperpigmentation occurs when there is an overproduction and/or erroneous distribution of melanin in the epidermis and/or dermis.
It is important to understand that every hyperpigmentation condition has slightly differing pathophysiologies. They all deal with melanin, but will differ in areas such as which skin layer the melanin is deposited in, which cells hold on to the melanin, and the processes which led to the erroneous production and/or distribution of the melanin in the first place. It is important to understand that because of this, not all dark spots can be treated the same.
Risk factors can be divided into fixed and variable risk factors. Fixed risk factors include our genetics/age/ethnicity and to some extent, hormonal changes. Variable risk factors are those we can change such as the amounts of UV exposure, heat, certain medications/sensitising agents or preventing a flare of an underlying inflammatory skin condition.
Genetics is one of the most essential variables to examine when determining why some people are more prone to developing hyperpigmentation than others.
Melanin production is controlled by genes inherited from our parents, resulting in varying skin tones due to varying types, amount and arrangement of melanin.
Genetic variations such as the MC1R gene variation is largely responsible for the development of freckles in caucasian and asian people when exposed to UV radiation.
People of different ethnicities possess varying levels of melanin in their skin. Those with darker skin tones typically have greater quantities, and darker types melanin, this protects them from sun damage such as sunburns, but also makes them more susceptible to hyperpigmentation changes such as melasma and post-inflammatory hyperpigmentation.
Conversely, fair-skinned individuals who have lower and lighter types of melanin, are more prone to sunburn and are less prone to such hyperpigmentation changes.
As we age, our skin undergoes several changes that can impact pigmentation. It is important to distinguish between normal skin ageing (Which happens regardless of UV exposure) and photoaging which occurs as a result of exposure to UV Radiation.
In fact as we age, the skin gets thinner and we lose melanocytes, thus actually contributing to more translucent and paler skin.
However older patients also suffer from more photoaging due to years of UV exposure. Those changes will be discussed in a later section.
Hormonal changes can also affect pigmentation. Common hormonal causes include fluctuations in oestrogen levels [often affected by pregnancy/menopause/medications].
1. Pregnancy
Hormonal changes, particularly increased levels of oestrogen and progesterone, play a role in the development of melasma, a skin pigmentation condition. These hormones stimulate melanocytes to produce more melanin, leading to the characteristic “mask of pregnancy” or Chloasma
2. Birth Control Pills
Synthetic hormones contained in birth control pills can lead to increased melanin production. If you experience skin changes while on hormonal contraceptives, discussing alternative options with your healthcare provider may be necessary.
3. Menopause
Menopause marks a significant hormonal transition for women as oestrogen levels decline. Some may experience improvements in hyperpigmentation conditions such as melasma, while others may get worsening of melasma especially in regions not on the face.
4. Other Hormones [Stress Hormones and Thyroid Hormones]
A myriad of other hormones can also contribute to hyperpigmentation through complicated mechanisms.
Prolonged sun exposure can make you more susceptible to developing hyperpigmentation.
Commonly known is the effect of UV Radiation on photo-ageing. UV Radiation can be split into UVA-1/UVA-2, UVB and UVC.
UVC is completely blocked off by the earth’s atmosphere.
UVAs and UVB all contribute to sunburns, hyperpigmentation, photoaging and skin cancers. However UVA rays have a higher propensity to darken the skin by penetrating the skin’s deeper layers where they stimulate melanocytes to produce melanin. On the other hand, UVB rays primarily affect the skin’s upper layers, causing immediate damage to the DNA within skin cells, leading to more sunburns.
It is thus important to practise sun avoidance and proper sunblock techniques to protect the skin from UVA and UVB.
Not too long ago, visible [blue] light has also been shown to increase the risk of hyperpigmentation and is the source of much discussion now.
Inflammation is often signalled by the presence of redness, heat, pain, swelling at the affected area. This is the body’s natural defence mechanisms against things like injury/infections whereby it sends chemical signals and cells to defend against these insults. Common causes of skin inflammation include acne, psoriasis, eczema, trauma and infections.
In this process, inflammatory mediators are released, which apart from fighting the insult, also contribute to increased melanin production by the melanocytes in the skin. Often in mild reactions, these are focused more on the surface of the skin and can easily be improved.
However, in the event of more serious inflammation/prolonged inflammation, there can be damage to the basement membrane of the epidermis. This causes the melanin produced to leak into the deeper layers of the skin where they are consumed by white blood cells. These can last in the skin for years and may need more intensive treatment to remove such as lasers/microneedling/stronger topicals.
Pigmentation changes caused by inflammation or trauma may not become apparent immediately. It can take days or weeks for the skin to respond to the inflammatory process or healing, and pigmentation issues may only manifest later.
There are many medications both topical and oral which can contribute to skin pigmentation. It is beyond the scope of this piece to discuss which medications. Some common examples are medications for arrhythmia, chemotherapy drugs, hormonal medications including the oral contraceptive pill, antibiotics and mental health medications amongst many others. These should be discussed with your healthcare provider to choose the most suited therapy for you. Please do not cease medications previously prescribed unless discussed with a healthcare professional.
Some common topical products can also cause skin irritation and post-inflammatory hyperpigmentation. One common example are retinoids for acne.
Having pigmentation can be frustrating, but there are pigmentation removal treatments available in Singapore to reduce its appearance and help restore your skin’s even tone.
It is vital to understand that not all hyperpigmentation can be treated the same. There are many diagnoses, each with very different causes and treatments.
Some overarching principles remain though
Here are some of the many treatment options used to improve pigmentation.
Pico pigmentation laser treatment also targets pigments like melanin or tattoo ink with ultra-short pulses of laser energy, breaking them down into tiny fragments that the body can remove naturally.
Pico lasers provide a multitude of benefits and are popular for addressing various pigmentation concerns, including age spots, freckles, melasma, tattoo removal and many more
RF Microneedling involves injecting the skin with many gold microneedles which release radiofrequency energy. This helps to prevent hyperpigmentation by improving the skin’s health from the source. It regulates melanocyte activity, strengthens a damaged basement membrane, removes abnormal vasculature and activates dormant fibroblast [Cells that produce collagen]. All in all this helps to improve the skin’s health and reduce the production of new pigment to stain the skin.
Often works very well when combined with PICO to remove the existing pigmentation quickly, while RF Gold Microneedling works to reduce further production of pigment.
Ethosome Gold PTT is a novel method of drug delivery, utilising ethosomes, soft malleable carriers to bring in medications to the deeper layers of the skin. Gold nanoparticles are also added for its proven anti-bacterial, anti-inflammatory and rejuvenation effects. In particular, the Brightening Ethosome Gold PTT, delivers Ethyl Ascorbyl Ether (antioxidant); Oral Medication for Pigmentation (amino acid for hyperpigmentation); niacinamide amongst other ingredients to assist with pigmentation.
There are many lightening agents in the market, of these, Depigmentation Cream is one with very well supported medical evidence.
Depigmentation Cream controls the activity of tyrosinase, an enzyme required in the steps for melanin production.
A 12-week study revealed that 79% of the subjects who received Depigmentation Cream had an improvement in pigmentation.
Depigmentation Cream is commonly used in combination with other medications but this should always be done under the guidance of a professional, as prolonged or excessive use can irritate skin or cause a rebound in hyperpigmentation.
What makes you susceptible to hyperpigmentation is a complex interplay of the above factors. While genetics and inherent traits are hard to avoid, our choices and exposures in life can significantly influence the development and severity of pigmentation concerns.
If you are suffering from pigmentation, there are several methods for pigmentation removal in Singapore, and consulting with a professional will determine which one is best for you.
Contact SL Aesthetic Clinic today to talk with one of our doctors and learn more about our prices and pigmentation removal treatments.
Like what you read? Share them!

Not sure if this treatment is right for you? Speak with our team in a no-obligation consultation, and view real patient results.